By Anne Mullens
When a routine screening test for colon cancer found blood in her sample earlier this year, Sherilyn Redekopp, of Campbell River, wasn’t too worried.
She’d had friends have similar results of their FIT (fecal immunochemical test) and their colonoscopies came back clear.
She had been feeling great, with no symptoms. So she prepped for the colonoscopy with no worry or concern.
“I didn’t think anything was going to happen,” she says.
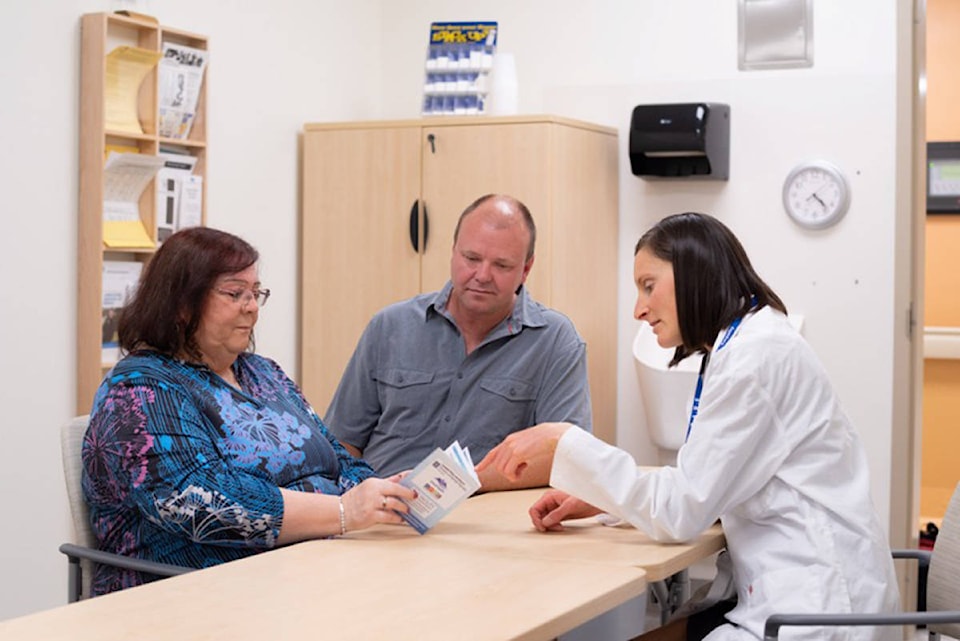
During the procedure, however, general surgeon Dr. Leanne Wood found concerning polyps, removing three at the time to send to pathology for closer examination.
When Redekopp emerged from the sedation Dr. Wood told her “I am 95 per cent sure they are malignant. You will be needing surgery” which the pathologist confirmed by the end of the week.
What could have been for many an anxious uncertain time — knowing you have cancer, waiting two weeks for surgery, having a major operation, and then recovering — was instead a time where Redekopp felt reassured and supported by her entire medical team. And where she felt that she was a fully-fledged, engaged partner in her own care and recovery.
“It could not have been a better process,” says Redekopp. “My husband and I were just amazed with everything that was done to get me ready and to ensure my recovery from surgery.”
That’s because Redekopp was part of a new surgical program that has been underway in Campbell River to improve surgical outcomes for patients. The project is an initiative of the Campbell River and District Division of Family Practice, supported in partnership by Doctors of BC and the BC government through the Shared Care Committee.
Around B.C,. and in other jurisdictions around the world, a process called Enhanced Recovery After Surgery (ERAS) is being adopted. This process includes more than 20 steps along a surgical journey, that research shows, significantly reduces complications, speeds healing, and shortens hospital stays. Dozens of locations around B.C. are adopting ERAS protocols for colorectal and other surgeries, with great results.
Campbell River, however, has taken the ERAS principles one step further — what they are calling ERAS Project Phase 2. Phase 2 expands the care team to include local family doctors as well as the surgical team, ensuring the patient is in the best possible shape before going into the operation, as well as supported coming out.
The initiative focuses on five areas: nutrition, exercise, stopping smoking, mental well being, and reversing anemia – all factors that can negatively affect surgery and recovery. To help guide the patient throughout the process, the patient receives a patient passport, and detailed handouts and guides provide education to keep patients informed every step of the way. Family doctors are key partners in supporting patients as they work through strategies to improve health before surgery as well as during recovery.
“Before this project, there was often a void, a disconnect, between the GPs and specialists. There was not a lot of planned communication —it was random,” explains Dr. Willem Prinsloo, who was the GP lead on the project. “This new project was all about creating pathways and protocols to have a system in place that keeps the GPs involved from diagnosis all the way through to recovery. It has really improved teamwork and communication —and that will improve the patient experience and patient outcome, maybe even increase life expectancy.”
“One of the main things we focused on was the patient experience,” said Dr. Wood, who was the specialist lead on the project. “When you hear you have cancer and you need an operation, you have to then wait two weeks. What can they do in those two weeks? We say, here, take this information. Here are the things you can be working on so you go into surgery in the best health.’ It is something positive they can focus on while getting ready for surgery.
For patients like Redekopp, ERAS protocols also have some key steps that patients are expected to take pre and post surgery. One item of information that surprised Redekopp, was the fact she would need to bring gum to the hospital, to chew after the operation to get her digestive track working again.
“I followed all the advice in the printed materials exactly as they told me,” says Redekopp “I did the leg exercises, the breathing exercises, and the chewing gum, even though I never usually chew gum. My goodness it kept me all so busy! It was incredible. I felt really supported, but I also felt that I was doing all I could, too, to have the best outcome,” said Redekopp.
Fortunately, her lymph nodes were clear and she did not need chemotherapy. By summer she was feeling almost 100 per cent, with only a slight tenderness in her incision.
Doctors in Campbell River are so happy with the results of the project, they will be keeping it in place indefinitely.
“The results were so positive for everyone that we are excited to keep it going,” said Dr. Wood.
Anne Mullens is a freelance health writer who works with the Shared Care Committee, a partnership of the Doctors of BC and the BC government.